flat back posture
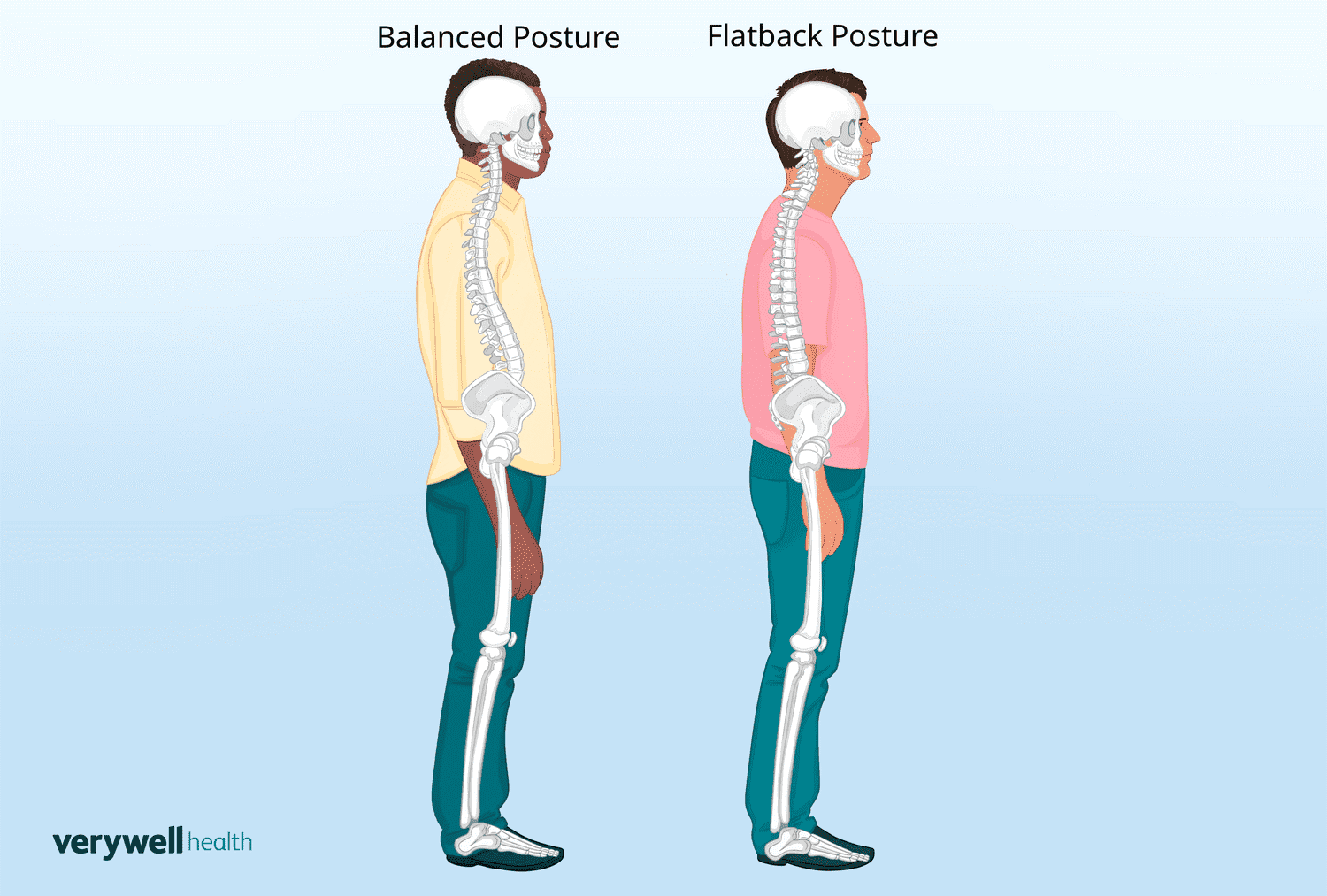
Flat back posture, or flatback syndrome, occurs when the natural inward curve (lordosis) of the lower back is reduced or absent. This imbalance can cause a person to lean forward, leading to chronic pain and difficulty standing upright. The spine's natural curves normally help to absorb stress and maintain balance.
Symptoms
Symptoms of flat back posture can vary but often include:
- Difficulty standing upright: You may feel as if you are falling forward, especially after standing or walking for long periods.
- Chronic pain: Pain may occur in the lower back, neck, hips, or thighs due to muscle fatigue from constantly trying to stay balanced.
- Stiffness: The muscles and joints in your lower back may become stiff and tight, making it harder to move.
- Fatigue: Muscles in the back and legs can become strained and tired more easily.
- Compensatory posture: You might compensate by bending your hips and knees or tilting your pelvis to maintain a more upright stance.
Causes
While poor posture is a contributing factor, other medical conditions can also cause flat back posture. Common causes include:
- Degenerative disc disease: The natural wear and tear of the spinal discs can lead to a loss of the lumbar curve.
- Spinal surgeries: Past surgical procedures, such as a laminectomy or spinal fusion, especially with older techniques like the Harrington rod, can flatten the spine.
- Ankylosing spondylitis: This inflammatory arthritis can cause the vertebrae to fuse and the spine to stiffen in a forward-flexed position.
- Vertebral compression fractures: Fractures, often related to osteoporosis, can cause a loss of height in the vertebrae and alter the spine's alignment.
- Muscle imbalances: Tight hamstrings and weak core or back muscles can pull the pelvis backward, flattening the lower back.
How to fix flat back posture
The treatment approach depends on the severity and underlying cause. Corrective measures can include non-surgical options like exercise and physical therapy, and in severe cases, surgery.
Physical therapy and exercises
- Stretching: Targeted stretches for tight muscles, such as the hamstrings, hip flexors, and abdominals, can help correct the pelvic tilt.
- Strengthening: Exercises like planks, glute bridges, and the "superman" help strengthen the core, back, and buttock muscles to support the spine.
- Posture training: A physical therapist can teach you proper body mechanics for sitting, standing, and lifting to reduce strain.
Other non-surgical treatments
- Medication: Nonsteroidal anti-inflammatory drugs (NSAIDs) can be used to manage pain.
- Bracing: In some cases, a brace can help support the spine and improve alignment.
Surgical intervention
- Surgery may be necessary for severe cases that don't respond to conservative treatment.
- Procedures such as an osteotomy or spinal fusion can help restore the proper spinal curvature and correct the imbalance.
For a personalized treatment plan, it's best to consult a spine specialist or physical therapist. Would you like me to help you find a spine specialist or physical therapist in your area?
